Breast Lift Surgery in Bangalore
Breast lift surgery — medically called mastopexy — is one of the most consistently satisfying procedures in breast cosmetic surgery. It repositions the breast tissue, removes the excess skin envelope, and places the nipple and areola at their natural height on the chest wall. When the size is right but the position is not, mastopexy alone is the appropriate answer. When both size and position need addressing, a combined augmentopexy (lift with implant) or reduction mastopexy (lift with reduction) is planned.
At Pink Apple Aesthetics, Jayanagar, breast lift surgery is performed by Dr. Pinky Devi Ayyappan, MCh (Plastic Surgery) — a female, board-certified plastic and reconstructive surgeon with 12+ years of experience and international fellowship training in Belgium, Seoul, and Italy. Breast ptosis assessment, technique selection, and the critical decision of whether a lift alone or a lift plus volume change is the right plan — these are the consultations that define the outcome, and they are conducted by Dr. Pinky herself.
What Is Breast Lift Surgery (Mastopexy) and What Can It Achieve?
Mastopexy is the surgical procedure that lifts and reshapes a sagging breast by removing excess skin, repositioning the breast tissue higher on the chest wall, and relocating the nipple and areola complex to a more youthful, natural height. It does not significantly change the size of the breast — it changes the position and shape.
As the breast ptoses (descends) over time, several changes occur simultaneously: the skin stretches and loses elasticity, the breast tissue itself descends below the crease beneath the breast, the nipple moves progressively lower and eventually points downward, and the upper pole of the breast loses its fullness. Mastopexy reverses these changes in a systematic, planned way:
- Excess, stretched skin is removed — the skin envelope that is now too large for the breast tissue within it is excised and the remaining skin is tightened around the repositioned breast
- The breast tissue is reshaped and repositioned — the internal breast tissue is mobilised and advanced upward, restoring the rounded, projected contour of a lifted breast.
- The nipple and areola complex is elevated — moved upward to sit at or slightly above the breast fold on the chest wall, pointing forward rather than downward.
- Areola diameter is reduced if appropriate — stretched areolas can be reduced to a more proportionate size as part of the same procedure.
Also known as: mastopexy, breast lift surgery cost Bangalore, sagging breast surgery, breast ptosis correction, breast lifting surgery, breast reshaping surgery, breast lift after pregnancy Bangalore.
The Four Grades of Breast Ptosis — Which Grade Are You, and Why It Matters
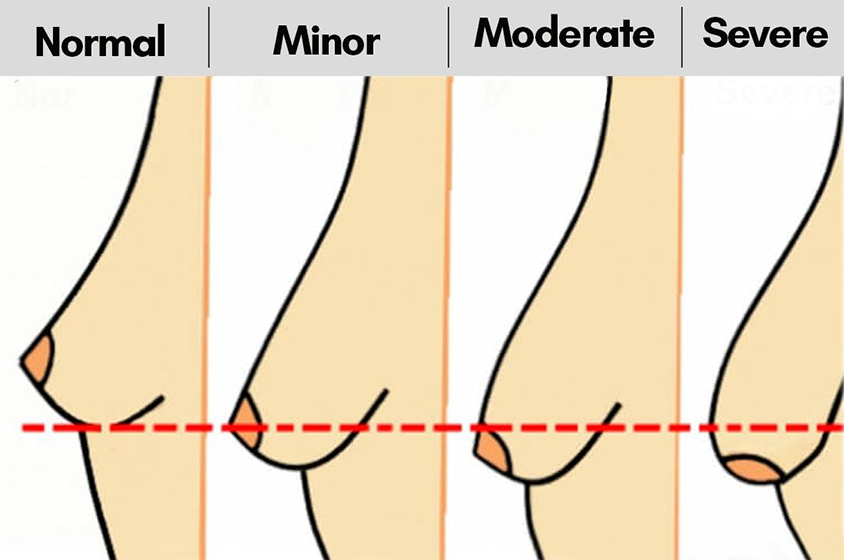
Breast ptosis is clinically graded using the Regnault classification, which measures the position of the nipple relative to the inframammary fold (the crease beneath the breast). This grading system directly determines which mastopexy technique is appropriate and how much correction is needed. Every patient consulting for breast lift should understand this grading — yet no Bangalore competitor explains it.
| Grade | Classification | What This Looks Lik | Technique Typically Needed |
|---|---|---|---|
| Pseudo-ptosi | Nipple above fold but breast tissue descends below it | Deflated upper breast; nipple appears well-positioned but breast hangs | Augmentation often alone; periareolar lift or crescent lift sometimes |
| Grade I (Mild) | Nipple at the level of the inframammary fold | Nipple just touching the lowest breast crease; modest sagging | Crescent or periareolar (donut) mastopexy |
| Grade II (Moderate) | Nipple 1–3 cm below the inframammary fold | Nipple clearly below the crease; visible drooping | Vertical (lollipop) mastopexy |
| Grade III (Severe) | Nipple more than 3 cm below fold; pointing downward | Significant sagging; nipple points down; majority of breast below fold | Anchor (inverted-T) mastopexy |
Knowing your ptosis grade is the most important step before any breast lift discussion. If you are unsure of your grade, a simple self-assessment is: can you hold a pencil horizontally under your breast crease and have it hold by the weight of the breast? If yes — you have at least Grade I ptosis. Dr. Pinky grades each breast individually at consultation because the two sides are often not identical.
Breast Lift Surgery Cost at Pink Apple Aesthetics
Breast lift surgery at Pink Apple Aesthetics starts from ₹1,00,000 to ₹1,50,000 (terms and conditions apply). Your confirmed cost is provided after a personal consultation with Dr. Pinky, once the ptosis grade, technique, and whether augmentopexy is needed have been assessed.
What your breast lift cost typically includes:
- Surgeon's fee — Dr. Pinky Devi Ayyappan, MCh Plastic Surgery.
- General anaesthesia and anaesthesiologist's fee.
- Surgical facility / operating theatre charges.
- One night of post-operative inpatient care
- Surgical bra — provided for the recovery period.
- Pre-operative blood tests and imaging.
- Post-operative medications — antibiotics and prescribed pain relief.
- Follow-up appointments — at 10 to 14 days (suture removal), 1 month, 3 months, and 6 months.
What affects the final cost:
- Technique — crescent/periareolar (simpler, less surgical time) vs vertical vs anchor (more involved, longer operating time).
- Grade of ptosis — more severe ptosis requires more extensive surgery
- Augmentopexy — if implants are being added alongside the lift, implant cost is added.
- Areola reduction — if included as part of the mastopexy, this is typically included in the procedure cost.
Breast lift surgery is a cosmetic procedure and is not covered by health insurance in most cases. EMI payment options are available at Pink Apple Aesthetics. If you are considering combined augmentopexy, the total cost will reflect both the lift and the implant components — these are discussed transparently at consultation.
Pseudo-Ptosis vs. True Ptosis — Why This Distinction Changes the Treatment Plan
Pseudo-ptosis is one of the most commonly misdiagnosed presentations in breast consultation — and correctly identifying it prevents patients from having surgery they don’t need, or from getting a lift when an implant would actually serve them better.
In pseudo-ptosis, the nipple position is normal — it sits at or above the inframammary fold. But the breast itself looks saggy, deflated, or empty, particularly in the upper pole. The breast tissue has not truly descended; it has simply lost volume. The skin envelope has become too large for the reduced breast content inside it.
This is extremely common in women post-breastfeeding or after significant weight loss. The breast looks droopy — but the cause is volume loss, not true descent of the nipple below the fold.
The implications for treatment are significant:
- True ptosis (Grades I–III) — requires mastopexy to reposition the nipple and remove excess skin. An implant without a lift will not correct the low nipple position.
- Pseudo-ptosis — may be fully corrected with breast augmentation alone (restoring volume fills out the skin envelope and recreates upper pole fullness). A lift may not be needed at all.
- Combined true ptosis with volume loss — requires both a lift and augmentation (augmentopexy). The lift corrects the nipple position; the implant restores the volume.
At Pink Apple Aesthetics, Dr. Pinky specifically assesses and explains this distinction at every breast consultation. Patients who present wanting a ‘breast lift’ often leave the consultation with a different — and better — understanding of what their specific anatomy actually needs. This honest assessment is the foundation of a result that matches expectations.
Mastopexy Techniques — Which Technique Is Appropriate for Your Grade of Ptosis?
The technique used for a breast lift is determined by the grade of ptosis. There is no single universally superior technique — the right approach is the one that matches the degree of correction needed to the incision pattern required. Choosing an insufficient technique for a higher grade of ptosis produces an inadequate result; choosing an over-invasive technique for mild ptosis creates unnecessary scarring.
1. Crescent Mastopexy (for very mild ptosis or nipple asymmetry adjustment)
A crescent-shaped incision is made at the upper border of the areola only. A crescent of skin is removed from above the areola, which elevates the nipple by 1 to 2 cm. This technique is only appropriate for very mild nipple asymmetry or minimal Grade I ptosis — it cannot lift the breast significantly and produces very limited reshaping. It is sometimes used in combination with augmentation when the nipple needs minor elevation alongside the volume addition. Scar: a fine line along the upper areola border, well concealed.
2. Periareolar (Donut) Mastopexy — for Grade I ptosis
Incisions are placed around the entire circumference of the areola. A donut-shaped ring of skin is removed, which draws the surrounding breast skin inward and upward, lifting the nipple by 2 to 4 cm. This technique also naturally reduces areola size. It is appropriate for Grade I (mild) ptosis and is the preferred approach when the patient also wants areola reduction. A permanent suture (purse-string suture) around the areola border prevents the areola from widening as healing occurs. Scar: a circular scar around the areola border — very well concealed at the pigment-skin transition.
3. Vertical (Lollipop) Mastopexy — for Grade II ptosis
The lollipop technique adds a vertical incision running from the areola downward to the breast fold, in addition to the periareolar incision. This combination allows more skin to be removed and more significant reshaping of the breast mound than the periareolar approach alone. The breast tissue is reshaped internally using parenchymal sutures that provide long-lasting breast shape. This is the most commonly used technique for moderate (Grade II) ptosis and for many post-pregnancy breast changes. Scars: periareolar scar + vertical scar from areola to fold (the 'lollipop' shape). Both scars are within the area covered by a bra.
4. Anchor (Inverted-T) Mastopexy — for Grade III ptosis
The most comprehensive mastopexy technique, adding a horizontal incision along the breast fold to the periareolar and vertical incisions. The anchor pattern allows maximum skin removal and the most significant breast repositioning — required for severe (Grade III) ptosis where the nipple points sharply downward and the majority of the breast tissue has descended below the breast fold. This technique is also used when mastopexy is combined with breast reduction. Scars: periareolar + vertical + horizontal fold scar (the 'anchor' or 'inverted-T' shape). All scars are within the area covered by a bra.
Scars from mastopexy are permanent but sit in positions that are hidden by all bras and swimwear. Modern suture techniques, silicone gel application from week 3, and consistent sun protection produce scars that fade to pale, inconspicuous lines within 12 to 18 months. For the majority of patients, the improvement in breast shape is worth the trade-off of the scar pattern — a decision Dr. Pinky discusses openly at consultation.
Augmentopexy — Breast Lift Combined with Implants: When Do You Need Both?
Augmentopexy — the combination of mastopexy (lift) and breast augmentation (implant) in a single surgical session — is one of the most requested breast procedures in cosmetic surgery. Understanding when you need both, and what the additional complexities of combining them are, helps patients make an informed decision at consultation.
When augmentopexy is the right choice
Augmentopexy is appropriate when a patient has both a low nipple position (true ptosis) AND insufficient breast volume. After pregnancy and breastfeeding, many women experience both simultaneously: the breast has descended below the fold (requiring a lift) AND lost glandular volume (requiring an implant to restore fullness). Mastopexy alone in this patient lifts the breast but leaves it looking small; augmentation alone adds volume but does not correct the low nipple position. Both together — augmentopexy — addresses both problems in a single procedure.
The surgical complexity of augmentopexy
Augmentopexy is technically more complex than either lift or augmentation performed alone. The competing tensions of the two procedures must be balanced: the lift requires skin tightening and tension across the closure; the implant requires adequate skin to accommodate it without excessive tension. Too much tension increases scar width and complications; too little leaves the lift inadequate. The nipple blood supply must be maintained through the lift while the implant sits beneath. Because of this complexity, some experienced surgeons prefer to stage augmentopexy — performing the lift first, allowing 3 to 6 months of healing, then adding the implant in a second session. Others perform both in one session when anatomy permits. Dr. Pinky will discuss with each patient whether a single combined session or a staged approach is more appropriate, based on the degree of ptosis, skin quality, and implant size desired.
Which implant and which lift technique for augmentopexy?
Typically, a moderate-profile round silicone implant is chosen for augmentopexy — providing upper pole fullness that the post-lift skin can accommodate without undue tension. The lift technique is chosen based on the grade of ptosis. Most augmentopexy procedures use a vertical or anchor lift pattern, as these grades of ptosis are the most common in the patients who also need augmentation.
A note on ‘just an augmentation will lift my breasts’: breast augmentation alone does not correct true ptosis. If the nipple is below the inframammary fold before augmentation, it will remain below the fold after — just with a larger breast. An implant without a lift for a patient with Grade II or III ptosis produces a ‘Snoopy breast’ or ‘rock in a sock’ appearance — widely recognised as a poor aesthetic outcome. Dr. Pinky will assess your ptosis grade at consultation and advise honestly on whether augmentation alone, lift alone, or augmentopexy is the correct approach.
Breast Ptosis in India — Post-Pregnancy, Breastfeeding, and What Indian Women Experience
India has a high breastfeeding rate — one of the highest in the world — and extended breastfeeding duration is culturally normative. Multiple pregnancies within a relatively short interval are also more common in India than in many Western countries. The combination of repeated pregnancy-related breast volume increase and decrease, extended breastfeeding, and the natural ageing process means that breast ptosis is a very common concern for Indian women in their 30s and 40s.
Specific characteristics of post-pregnancy breast ptosis in Indian women:
- Volume deflation is often more significant than descent — many Indian women present with pseudo-ptosis or Grade I true ptosis combined with significant volume loss, rather than the severe Grade III descent seen in older patients or those with very large pre-pregnancy breasts. For these patients, augmentopexy or augmentation alone may be the most appropriate approach.
- Skin elasticity considerations — Indian skin has higher collagen density in youth but can thin significantly after multiple pregnancies. The quality of the remaining skin after breastfeeding affects which technique will hold the lift result most durably.
- Timing after breastfeeding — it is recommended to wait at least 6 months after completing breastfeeding before proceeding with mastopexy. This allows the breast to fully involute (return to its resting state) — the breast continues changing for several months after breastfeeding ends, and operating too early gives an inaccurate picture of the final ptosis degree.
- Future pregnancies and the longevity of results — future pregnancy after mastopexy will affect the breast again. While surgery does not prevent future pregnancies, most surgeons recommend that patients complete their family before undergoing breast lift surgery, as another pregnancy significantly changes breast shape and size.
Dr. Pinky treats a large proportion of patients in this exact demographic — Indian women post-breastfeeding who want to reclaim their breast shape. The consultation is conducted with understanding of this specific context, and the treatment plan is designed to produce a long-lasting result appropriate to the patient’s life stage.
Who Is a Good Candidate for Breast Lift Surgery?
- Visible breast ptosis — the nipple sits at or below the inframammary fold; the breast tissue has descended below the crease; the upper breast has lost its fullness and projection.
- Nipple that points downward or outward — rather than forward; an early sign of progressive ptosis that responds well to mastopexy.
- Stable weight for at least 6 months — weight change significantly affects breast shape. We recommend stable weight for at least 6 months before the procedure.
- Completed breastfeeding — and waited at least 6 months after weaning so the breast has fully involuted.
- Not planning further pregnancies — ideally. Future pregnancy will affect the result of a breast lift. Patients who may become pregnant again should factor this into the timing of their decision.
- Non-smoker or committed to stopping — smoking significantly impairs wound healing and is a particular risk factor for nipple and skin flap complications in mastopexy.
- Good general health — no uncontrolled conditions affecting surgical safety.
- Realistic expectations — mastopexy significantly improves breast position and shape. It does not make breasts larger, prevent future natural ageing, or guarantee permanent results independent of lifestyle factors.

Breast lift surgery produces the most durable results when combined with a stable weight and a healthy lifestyle. Large weight fluctuations after mastopexy will affect the result over time, as they affect all breast tissue.
What to Expect: From Consultation to Your Result
Step 1 — Consultation and ptosis assessment
Dr. Pinky examines both breasts individually — assessing ptosis grade, nipple position relative to the inframammary fold, skin quality and elasticity, areola size, breast volume, and the presence of any asymmetry. She takes standardised photographs and uses these to discuss the planned technique, the expected scar pattern, and whether augmentopexy or mastopexy alone is the right recommendation. She sets honest expectations about results, scars, and the impact of future pregnancies.
Step 2 — Pre-operative preparation
Blood tests and medical assessment. Baseline breast imaging for patients over 35 or with family history of breast cancer. Stop smoking at least 4 to 6 weeks before surgery. Stop blood thinners and relevant supplements 1 to 2 weeks before. Surgical markings are drawn while standing — pre-operatively, not after anaesthesia — for maximum precision.
Step 3 — The surgery (2 to 3 hours)
Mastopexy is performed under general anaesthesia. Standalone mastopexy takes 2 to 3 hours. Augmentopexy takes 2.5 to 3.5 hours. Most patients are admitted for one night and discharged the following morning. The breast tissue is repositioned and reshaped according to the planned technique, the nipple is elevated to its new position on the pedicle, excess skin is removed, and the wound is closed in layers with fine sutures.
Step 4 — Recovery: first two weeks
A supportive surgical bra is worn day and night for 4 to 6 weeks — this is the most important garment in post-mastopexy recovery and should be worn consistently. Drains may be used for 24 to 48 hours. Significant swelling and bruising is expected for the first 1 to 2 weeks and gradually resolves. Most patients return to desk work and light activity within 1 to 2 weeks. Arm-raising above shoulder height and heavy lifting should be avoided for 4 to 6 weeks.
Step 5 — Weeks 3 to 12
By week 3, most patients are socially presentable and clearly see the improvement in breast position and shape. Scars are pink and slightly raised in the first 3 months. Medical-grade silicone gel on the scars from approximately week 3 accelerates fading. Exercise and strenuous activity resumes at 6 weeks. The breast continues to soften and settle over 3 to 6 months.
Step 6 — Your final result
The final, fully settled result is visible at 3 to 6 months when all swelling has resolved and the breast tissues have adapted to their new configuration. The result is long-lasting — most patients maintain the improvement for 7 to 10 years with stable weight. Ageing and gravity continue to act on the breast, but from a significantly improved baseline.
What Are the Risks of Breast Lift Surgery?
- Scarring — permanent scars are an unavoidable outcome of mastopexy. They are positioned within the area covered by all bras and swimwear and fade significantly over 12 to 18 months with silicone gel and sun protection. For most patients, scars are an entirely acceptable trade-off for the improvement in breast position.
- Altered nipple and breast sensation — temporary changes in nipple sensation are common as the nerve supply adjusts to the new nipple position. Sensation typically returns over 3 to 12 months. Permanent sensory change is uncommon.
- Wound healing complications — particularly at the T-junction where the vertical and horizontal scars meet, in patients who smoke or have compromised circulation. Smoking cessation before surgery is non-negotiable.
- Nipple or skin necrosis — the most serious complication of mastopexy; occurs when blood supply to the nipple pedicle is compromised. Risk is significantly elevated in smokers, patients with diabetes, and in very large breast lifts. Careful pedicle design minimises this risk.
- Asymmetry — minor asymmetry during healing is normal and expected. Significant asymmetry requiring revision is uncommon with careful pre-operative planning and bilateral measurement.
- Loss of lift over time — gravity and natural ageing continue to act on the breast after mastopexy. The result is long-lasting — most patients maintain the improvement for 7 to 10 years — but is not permanent. Future pregnancies, significant weight gain, or natural ageing will affect breast position over time.
- Haematoma and seroma — uncommon; managed with aspiration or surgical drainage if they occur.
- Infection — uncommon; managed with antibiotics and wound care.
- Breastfeeding impact — mastopexy, like all breast surgery, may affect breastfeeding potential. Most techniques preserve the nipple pedicle with its milk duct connections. Breastfeeding is possible for most patients after mastopexy but cannot be guaranteed.
At Pink Apple Aesthetics, risk management begins with accurate candidacy assessment — particularly smoking status, weight stability, and whether future pregnancy is planned. Patients who are informed and well-prepared have the best surgical outcomes.
Before and After Procedures
Look At The Difference
Why Choose Dr. Pinky Devi Ayyappan for Breast Augmentation Surgery?
Female, board-certified MCh plastic surgeon
One of very few female MCh plastic surgeons in Bangalore. Breast lift surgery is intimate and personal — and for the majority of women, the consultation and the surgical decision-making process are significantly better when conducted by a female surgeon who brings both clinical authority and personal understanding.
MCh (Plastic, Reconstructive & Aesthetic Surgery)
India’s highest postgraduate plastic surgery qualification. Formal training in all mastopexy techniques — periareolar, vertical, anchor, and combined augmentopexy.
Accurate ptosis grading at every consultation
Dr. Pinky uses the Regnault classification to grade each breast individually before making any technique recommendation. The correct technique is selected by the anatomy, not by a standard approach applied to everyone.
Pseudo-ptosis vs true ptosis distinction
Dr. Pinky specifically assesses whether volume loss or true nipple descent is driving the ptosis appearance — because this changes the entire treatment plan. Many patients who think they need a lift actually need an augmentation; some need both.
DAFPRS Fellowship — Belgium (Dr. Patrick Tonnard & Dr. Alexis Verpaele)
International training with globally recognised plastic surgeons.
Facial Aesthetic Surgery Fellowship — Seoul
Additional international surgical training
4.9 stars from 191+ verified Google reviews
Consistent, trusted patient outcomes.
Times of India Top Brand 2024
Recognised among Bangalore’s leading aesthetic clinics.

Breast Lift Surgery — Frequently Asked Questions

What is the difference between a breast lift and breast augmentation?
A breast lift (mastopexy) addresses the position of the breast — it lifts a sagging breast upward, corrects a low nipple, and reshapes the breast contour. It does not significantly change breast size. A breast augmentation adds volume using an implant — it makes the breast larger but does not correct a low nipple position. If your nipple is below the breast fold, an augmentation alone will not lift it — you will need a mastopexy. If the breast size is right but the position is wrong, a mastopexy alone is the answer. If both are needed, augmentopexy (lift + implant) is the combined procedure.
Do I need a breast lift or will an implant lift my breasts?
This depends entirely on your ptosis grade. If your nipple is at or below the inframammary fold (the crease beneath the breast), augmentation alone will not correct the nipple position — you need a lift. If your breast appears saggy primarily because of volume loss (the skin envelope is too large for the tissue inside it), this is pseudo-ptosis — and augmentation alone may give you the improvement you want without a lift. Dr. Pinky assesses this specifically at consultation. Many patients who come in expecting to need a lift find that augmentation alone is the right answer; others who thought augmentation would suffice learn they also need a lift. Accurate assessment protects both the result and the investment.
How long does a breast lift last?
A breast lift provides long-lasting improvement — most patients maintain the result for 7 to 10 years with stable weight. The ageing process continues after surgery, but from a significantly improved baseline. Factors that reduce longevity of results: significant weight gain after surgery, subsequent pregnancies, and skin elasticity at the time of surgery. Maintaining stable weight and wearing a supportive bra consistently are the most important patient-side factors in preserving the lift result over time.
Will I be able to breastfeed after a breast lift?
In most cases, yes. The standard mastopexy technique preserves the nipple on a pedicle of breast tissue that includes the major milk ducts — meaning the connection between the milk-producing glands and the nipple is maintained. Breastfeeding is possible for most patients after mastopexy. However, it cannot be guaranteed — some patients experience reduced milk production or difficulty with latch. If breastfeeding future children is a priority, discuss this specifically with Dr. Pinky so the technique and pedicle design can be planned with this in mind.
What are the scars from a breast lift like?
The scar pattern depends on the technique. A periareolar lift leaves a circular scar around the areola. A vertical lift adds a vertical scar from the areola to the breast fold. An anchor lift adds a horizontal scar along the breast fold. All scars sit within the area covered by a bra or bikini top — they are not visible in normal clothing or swimwear. Scars appear pink and raised in the first 3 months and gradually fade over 12 to 18 months with silicone gel and sun protection. Most patients find the scars entirely acceptable given the dramatic improvement in breast shape and position.
Can I have a breast lift and get implants at the same time?
Yes — this is called augmentopexy and is performed in a single surgical session. It is appropriate for patients who have both true breast ptosis (low nipple) and insufficient breast volume. The lift corrects the nipple position; the implant restores the volume. Augmentopexy is technically more complex than either procedure alone, and for patients where the degree of ptosis is very significant, a staged approach (lift first, implant 3 to 6 months later) may be recommended for the safest outcome. Dr. Pinky will discuss both options at consultation.
Should I wait until after my last pregnancy before having a breast lift?
Ideally, yes. Future pregnancy will significantly affect the breast again — volume increases during pregnancy, changes again during breastfeeding, and the breast often re-ptoses as a result. Having a breast lift before completing your family means the result may be significantly altered by a future pregnancy. That said, there is no medical danger in becoming pregnant after mastopexy, and some women in specific life circumstances choose to proceed knowing this. Dr. Pinky will discuss the timing question honestly in the context of your plans at consultation.